What is Muscular Dystrophy?
Muscular Dystrophy is a heterogeneous group of inherited disorders and more often presenting in childhood. The progressive degeneration or degradation of muscle fibers leads to muscle weakness and wasting.
Types of Muscular dystrophy
- X-linked muscular dystrophy:
- Duchenne muscular dystrophy
- Becker muscular dystrophy
- Autosomal muscular dystrophies:
- Limb-girdle muscular dystrophies
- Facioscapular humeral muscular dystrophy
- Oculopharyngeal muscular dystrophy
- Myotonic dystrophy
Duchenne muscular dystrophy (DMD)
It is an inherited progressive myopathic disorder and the X-linked recessive form of muscular dystrophy & affects 1 in 3600 boys. It caused by the absence of dystrophin due to frameshift mutations in the dystrophin gene and hence is termed “dystrophinopathy”.

Pathogenesis
It is caused by mutations of the dystrophin gene located on chromosome Xp21.2 and the deletions of around 72% of patients. The partial gene duplications around 6 – 10% of patients. The point mutations in the coding sequence or the splicing sites.
Dystrophin protein is mostly found in skeletal and cardiac muscles. Dystrophin is a part of the dystrophin-glycoprotein complex and Dystrophin-glycoprotein complex damage results in an influx of ca++ ions.
Muscle cell membrane damage associated with the loss of dystrophin may permit the pathologic entry of extracellular calcium into muscle fibers. The excess cytosolic calcium ion can activate calpains, which promote muscle proteolysis.
The results in degeneration and regeneration of muscle fibers and finally leads to muscle fibers are replaced by connective fibrous tissue and adipose tissue.
Clinical Features
- Normal at birth, Onset of various symptoms by age 5.
- Waddling gait (Duck like)
- Wheelchair-bound by age 10
- Proximal weakness of the shoulder and pelvic girdles
- Calf pseudo-hypertrophy (in the muscles replaced by fat & connective tissue)
- Heart failure and arrhythmias may occur.
- Respiratory insufficiency and pulmonary infections
- Death because of respiratory failure by the second or third decade of life
Gowers Sign
A patient uses his hands and arms to “walk” up his own body from a squatting position due to a lack of hip and thigh muscle strength. A patient with Duchenne muscular dystrophy (DMD) demonstrating the Gowers maneuver.
- The prone position.
- The bear position.
- Moving the hands up the thighs with help upright the trunk and augment knee extension.
- The upright position.
Diagnosis of the muscular dystrophy
The diagnosis of a dystrophinopathy is suspected based on the following features:
- Characteristic age and sex.
- On the basis of the presence of signs & symptoms suggestive of a myopathic process.
- Markedly increased serum creatine kinase values.
- Myopathic changes on electromyography and muscle biopsy.
- A positive family history suggesting X-linked recessive inheritance disorder.
- Immunostain: Decreased dystrophin protein
- PCR: DNA analysis
Serum muscle enzymes
- Markedly raised serum Creatine Kinase (CK) level, 10-20 times the upper limit of normal.
- Levels peak at 2-3 years of age and then decline with increasing age, due to progressive loss of dystrophic muscle fibers.
- Elevated serum ALT, AST, aldolase, and LDH.
Electromyography (Needle electromyography)
- Short duration, low amplitude polyphasic motor unit potentials in proximal muscles site.
- Over time, some of these areas become electrically silent when electromyography is done.
Muscle biopsy
- The gold standard for diagnosis
- Performed when genetic testing is negative (-ve), or the clinical phenotype is atypical nature.
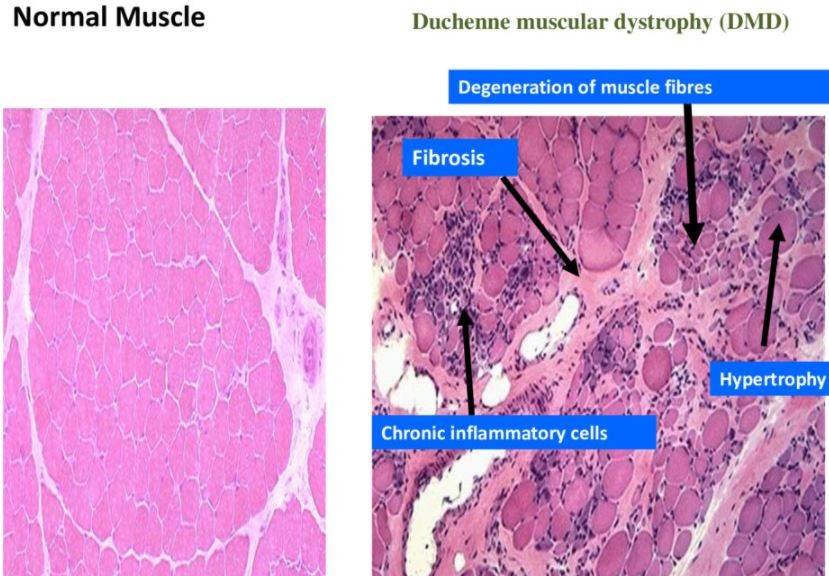
Morphology
- Muscle fibers of various sizes
- Necrosis, degeneration, and regeneration of fibers
- Fibrosis Fatty infiltration
Becker’s muscular dystrophy
It is less common but not as severe as Duchenne’s. It is a mutation that produces an altered dystrophin protein. Later onset with variable progression. Cardiac involvement is rare and may have a relatively normal life span.
Management
Cardiac disease
- Cardiac surveillance beginning at 10 years & continuing on a yearly basis.
- Early treatment of dilated cardiomyopathy with ACE inhibitors agents and beta-blockers agents.
- Improvement in Left Ventricular function
Respiratory disease
- Baseline pulmonary function tests & respiratory evaluations beginning at age 8 years to 9 years.
- Pneumococcal vaccine and annual flu vaccination.
- Acute respiratory deteriorations due to the fact that infections require early management with antibiotics, chest physiotherapy, and respiratory support.
- Nocturnal non-invasive intermittent positive (+ve) pressure ventilation (NIPPV) for a condition called hypercapnia.
Orthopedic problems
- Passive stretching
- Night splints
- Surveillance radiographs for scoliosis
- Maintenance of bone density
- Monitoring of vitamin D levels & supplementing calcium elements & vitamin D.
Corticosteroid Therapy
- Prednisolone drug, prednisone, & deflazacort have been the only drugs shown to be effective or fruitful to date in DMD.
Gene Therapy