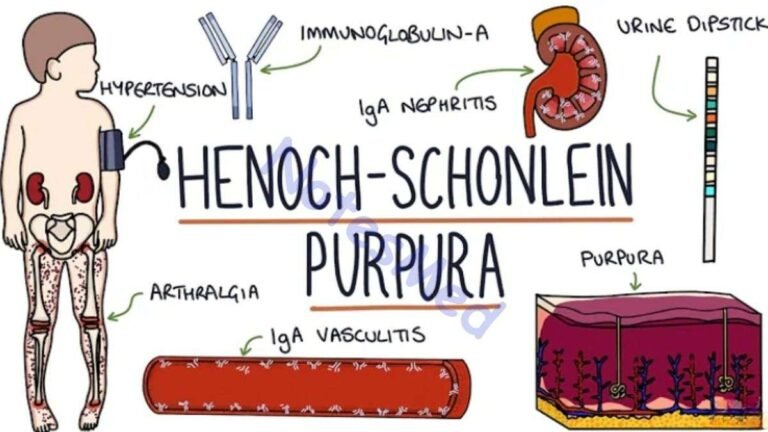
What is hypercalcemia?
Hypercalcemia is the most common metabolic disorder in patients with cancer and has a prevalence of 15-20 cases per 100000 persons and in which the calcium level in blood is above normal.
The incidence is highest in breast cancer and myeloma (approx. 40%), non-small cell lung cancer, and uncommon in the colon, small cell lung carcinoma, and prostate.
The hypercalcaemia level is more than 11 mg/dl of calcium present in the blood in your body.
It is generally due to the overproduction of PTHγP, which binds to the PTH receptors and elevates serum calcium by stimulating osteoclastic bone resorption and increasing renal tubular reabsorption of calcium levels.
Calcium is an important mineral in our bodies throughout our lifetime for bone growth and development, bone strength, maintaining proper hormone levels, and optimal functioning of nerves, the brain, and muscles in our body.
The normal level of calcium is maintained at 9-11 mg/dl. The biologically active calcium is an ionized fraction.
A normal adult human body usually has 20-25 gm of calcium/ Kg of body weight. The calcium level is usually very cautiously controlled by the human body.
Too much calcium in our blood can weaken our bones, create some kidney abnormalities like kidney stones, and interfere with heart and brain working activity.
Hypercalcemia can be a life-threatening condition in our human body and can result when too much calcium enters into the extracellular fluid (ECF) in the body or when there is an insufficient amount of calcium excretion from the kidneys. Around 90% of cases of hypercalcemia are caused by the malignancy of hyperparathyroidism.
What are the causes of hypercalcaemia (pathophysiology of hypercalcemia)?
- Hyperparathyroidism
- Malignancy
- Granulomatous Diseases
- Drug-induced Hypercalcaemia
- Overdose of Vitamins
- Hereditary factors
- Severe dehydration

Hyperparathyroidism
It is due to the increased activity of PTH that is responsible for the increase in the plasma concentration of calcium.
The increased level of PTH may be due to the following condition such as familial history, hyperplasia of parathyroid glands, parathyroid adenomas, and parathyroid carcinoma, etc.
Hypercalcemia of malignancy
Lung cancer and breast cancer, as well as some cancers of the blood (multiple myeloma), can increase the risk of hypercalcemia.
It may be due to activation of PTH-related protein (PTHγP), tumor growth factor, interleukin-1, etc. that stimulates the release of PTH and thus resulting in hypercalcemia.
Direct erosion of bone by a tumor may also lead to hypercalcemia. Production of prostaglandin (PGE2) by the tumor can produce bone resorption.
Drug-induced hypercalcemia
Some drugs like thiazide diuretics, lithium, etc. can cause hypercalcaemia. Thiazide diuretics drugs can increase renal tubular reabsorption of calcium resulting in hypercalcemia condition.
Lithium, which is used to treat bipolar disorder (manic-depressive illness), might increase the release of parathyroid hormone.
Granulomatous diseases
Tuberculosis, sarcoidosis, etc. can raise vitamin D levels in the blood in our body, which stimulates the digestive tract to absorb more calcium levels.
Overdose of vitamins: hypervitaminosis D
Taking excessive amounts of calcium or vitamin D supplements from different sources over time can raise the level of calcium in the blood above normal levels in our body.
Hereditary factors
A rare genetic disorder known as familial hypocalciuric hypercalcemia causes an increase of calcium in the blood because of faulty calcium receptors (calcium-sensing receptors [CaSR] in the body. This condition doesn’t cause any symptoms or complications of hypercalcemia.
Severe dehydration
The most common cause of mild or transient hypercalcaemia is dehydration which having less fluid in the blood can cause a rise in calcium concentrations in the human body.
Immobility
Immobility is another cause of hypercalcemia. Those people who have this type of condition that causes them to spend a lot of time sitting or lying down can have a more chance to develop hypercalcemia. Over time, bones that don’t bear weight and release calcium into the blood.
What are the symptoms of Hypercalcemia?
- Some common signs and symptoms of hypercalcemia are following below;
- Frequent urination and thirst
- Fatigue, headaches, bone pain
- Nausea, vomiting, constipation, decrease in appetite
- Forgetfulness
- Depression, memory loss or irritability, lethargy
- Muscle aches, weakness, cramping, and/or muscle twitches
How to diagnose and test hypercalcemia?
In the diagnosis of hypercalcemia, the most common test is hypercalcemia blood tests which determine calcium levels are elevated, and physicians or consultants will often review medications history as well as conduct a physical examination.
If there is no obvious cause, the physician or consultants may ask to see an endocrinologist, who will give you further hormonal testing such as parathyroid hormone (PTH) and Calcitonin.
What are the complications of hypercalcaemia?
There are chances to develop some common complications during or after hypercalcemia conditions or treatment time. There are the following complication explain briefly,
- Osteoporosis
- Kidney stones
- Nervous system problems
- Abnormal heart rhythm (arrhythmia)
Osteoporosis
If bones continue to release calcium into the blood, it can lead to a chance to develop osteoporosis resulting in bone fractures, spinal column curvature, and loss of height, etc.
Kidney stones
If the urine contains an excessive amount of calcium level, the crystals may form in the renal system such as the kidneys. Over time, the crystals may combine to form stones in the kidney which are called kidney stones.
Nervous system problems
Severe hypercalcemia conditions can lead to some clinical abnormalities in nervous systems such as confusion, dementia, and coma, which can be fatal.
Abnormal heart rhythm(arrhythmia)
Hypercalcemia can affect the electrical impulses that regulate heartbeat and cause the heart to beat irregularly (dysrhythmia).
What are the Hypercalcemia treatment guidelines?
There are some procedures for the management and treatment of this type of hypercalcaemia.
The management and treatment of hypercalcemia depend on the severity of the conditions. Some common hypercalcemia management outlines are following below,
- Drink more water that helps to excrete the excess calcium through urine.
- Switch to a non-thiazide diuretic drug or blood pressure medicine.
- Stop calcium-rich antacid tablets, which help to reduce calcium levels in our body.
- Stop calcium supplements (hypercalcemia diet cut out) such as dairy products, green leafy vegetables (curly kale, okra, and spinach, etc.), fish where they eat the bones (sardines and pilchards), etc. which help to reduce calcium levels in the body.
- Surgery to remove the overactive gland: in some conditions, there is the removal of overactive glands which helps to reduce calcium levels as well as reduce the chance to develop complications.
Medical management of severe hypercalcemia
There are some common medical management of severe hypercalcemia, which are following below;
- IV fluids for hypercalcemia (0.9% saline) 2-4 L/day
- Normal saline improves renal function and increases urinary excretion of calcium.
- Concurrently, intravenous bisphosphonates
- The IV bisphosphonates inhibit bone resorption, and usually, reducing the calcium levels to normal within 5 days, but if not normal level, then treatment can be repeated as soon as possible.
- Calcitonin for hypercalcemia (IM/SC)
- Calcitonin does for hypercalcemia acts rapidly to increase calcium excretion. The calcitonin reduces bone resorption so can be given combined with fluid and bisphosphonate therapy for the first 24–48 hours in patients with life-threatening hypercalcemia.