Overview of Rabies virus
Rabies virus causes a rapidly progressive acute infectious disease of the central nervous system in human beings as well as other animals, transmitted from another rabid animal.
It is worldwide distributed and infected many mammals including humans.
Classification of rabies virus
- Family-Rhabdoviridae
- Genus-Lyssavirus
- Species: Rabies lyssavirus
Street virus
It is immediately isolated from natural infection and produces Negri's body. It affects salivary glands which are pathogenic in nature.
The incubation period around 1-3 months and produce disease.
Fixed virus
It isolated after passing several times in the cerebrum of the rabbit and can’t produce Negri body.
The fixed virus doesn’t affect the salivary gland and its incubation period is 4-6 days and it used for vaccine.
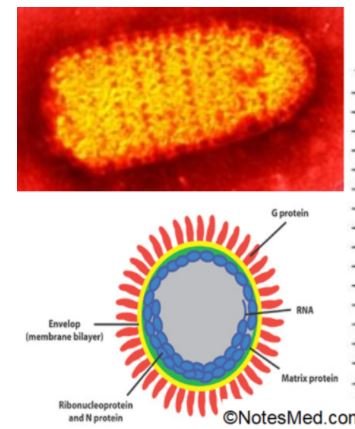
There are 5 types of viral proteins are present which are briefly described below;
- ‘G’ Surface protein: This is a surface glycoprotein and is a transmembrane protein. It targets neutralizing antibodies.
- ‘M’ Matrix protein: This is a peripheral membrane protein, lining the inner surface and acting as a bridge between ‘G’ protein & nucleocapsid.
- Nucleocapsid protein: It is an infectious ribonucleoprotein core at the center and helical structure that lies within the membrane. It protects the genome from nuclease enzymes.
- ‘L’ protein & ‘NS’ or ‘P’ protein: These viral proteins together form the RNA-dependent RNA polymerase. The ‘L’ protein’s molecular weight is 240 KDs, 60% of the genome.
Transmission of rabies virus & disease
Rabies virus usually transmitted to human beings by the bite of infected animals (rabid) like dogs, foxes, jackals, etc.
It is rarely by corneal or by other tissues (kidney, liver) transplantation and it is also transmitted by contact of infected saliva with mucous membranes or open wounds and also transmitted through the inhalation of aerosolized rabies virus – mainly in lab workers, bat caves.
Pathogenesis of rabies virus
Initially inoculation of the virus through the skin via various sources such as a dog bite. Then, replication within the striated muscle cell.
It then accesses the peripheral nervous system at neuromuscular and neuro-tendinous spindles. Now binds to nicotinic acetylcholine receptors & then penetrates nerve endings such as sensory and motor.
It spreads in a centripetal manner (nerve of CNS) through peripheral nerve axoplasm ( rate of nearly 3mm/hr).
It multiplies in the brain, cerebellum, and other brain structures causing diffuse encephalitis.
Finally, Passes centrifugally along autonomic nerves to other tissues(like salivary glands, adrenal medulla, kidneys, lungs, cornea, skin, etc.)
Clinical manifestations
- Incubation phase for 1-2 months( 7 days to years)
- The clinical spectrum can be divided into three phases such as;
- Prodromal (Non-specific): Fever, headache, malaise, myalgias, anorexia, nausea, vomiting (2-10 days)
- The clinical spectrum can be divided into three phases such as;
- Acute neurological phase (2-7 days):
- Either encephalitic rabies (80%) or paralytic rabies (20%).
- Coma and death ( survival and recovery are rare).
Encephalitic rabies
The signs of nervous system dysfunction such as nervousness, apprehension, and hallucinations.
Most patients have cardinal features of encephalitis hydrophobia, acrophobia, and fluctuating consciousness, difficulty in drinking.
Paralytic rabies
The paralytic rabies about 20% cases (mostly with bat rabies) are shown. The characteristic features are muscle weakness, the cardinal sign of rabies is lacking.
Early and prominent muscle weakness, quadriparesis, and facial weakness. The course of the disease is slower (up to 30 days survival).
Laboratory diagnosis
If overt symptoms present therapeutic intervention too late. It can be diagnosed either in man or animal should be different
Human diagnosis
There are two-stage of diagnosis such as antemortem and postmortem.
At Antemortem
The detection of rabies antigens or nucleic acids before death. The virus isolation is done on mouse inoculation and cell lines (mouse neuroblastoma cell lines and baby hamster kidney cell lines). The serology test should be done.
A Postmortem
The demonstration Negri bodies, isolation of virus after the death of patients. The antigen detection should be done by taking a skin biopsy (full-thickness from the nape of the neck including the base of hair follicles and also brain or corneal smears).
Isolation of virus: The isolation of virus should be done on mouse inoculation and cell line (mouse neuroblastoma cell lines and baby hamster kidney cell lines).
Negri bodies: It is an eosinophilic intracytoplasmic inclusions body (50-80% cases) with basophilic inner granules.
Antibody detection
The detection of CSF antibodies more significant but develop slowly. There are other different antibodies detection test such as;
- Mouse neutralization test (MNT)
- Rapid fluorescent focus inhibition test (RFFIT)
- Fluorescent antibody virus neutralization test (FAVN)
- Indirect fluorescence assay (IFA)
- Hemagglutination inhibition test (HAI)
- Complement fixation Test (CFT)
- Reverse transcription(RT)- PCR: sensitive
Animal rabies
In animal rabies, the detection from the brain biopsy 2 portions. one in 50% glycerol saline (for detection of antigen) and the other in Zenker’s fixative (for microscopy).
Tests in animal rabies
- Immunofluorescence test
- Demonstration of Negri bodies
- Isolation of virus
Immunofluorescence test
This is a highly reliable and the best single test that is available for the rapid diagnosis of rabies viral antigen in infected specimens.
This can establish a highly specific diagnosis within a few time. The examination of salivary glands is most useful.
Further, fluorescent antibody titers in clinical rabies have been well in excess of 1:10,000, a feature that helps to distinguish between rabies and vaccine reaction.
Prophylaxis of rabies virus
- Pre-exposure prophylaxis: It is only in persons at high risk(immunization)
- Post-exposure prophylaxis:
- Wash the wound immediately with soap & water.
- Treat with alcohol or an antiseptic.
- If an animal available then strict isolation and close observation have to be done.
- Start vaccination
Vaccines
- Neural vaccines
- Non-neural vaccines
- Subunit vaccine: surface glycoprotein cloned (in experimental stage).
Neural vaccines
It was prepared by Louis Pasteur in 1885 and modified later. It is poor immunogens& a serious risk of neurological complication, postvaccinal encephalitis after vaccination. For example;
- Semple vaccine: It is derived from infected sheep brain, and inactivated with phenol.
- Betapropiolactone( BPL) vaccine: It is a modified semple vaccine and inactivated with beta propiolactone instead of phenol
- Infant mouse brain vaccines: This vaccine was derived from infected neural tissue of newborn mice.
Non-neural vaccines
The non-neural vaccine includes recombinant glycoprotein, egg-derived, and cell line-derived vaccines.
Egg vaccines
- Purified duck egg vaccine (poor immunogenicity and less reactogenic hence multiples doses have to be given).
- Live attenuated chick embryo vaccines (not suitable for humans).
Tissue culture vaccines
- Human diploid cell vaccine (HDCV): derived from WI-38.
- Purified chick embryo cell (PCEC) vaccine: derived from chicken fibroblast cell line.
- Purified Vero cell ( PVC) vaccine.
Passive immunization
- Equine rabies immunoglobulin ( ERIG)
- Human rabies immunoglobulin ( HRIG)
It is recommended when exposure is at high risk like the bite is above the neck region.
Vaccination schedule
Cell culture vaccines
- Pre-exposure
- 3 doses ( 0,7,21 or 0,28, 56 days), booster after 1 year.
- Post-exposure
- 5 or 6 doses ( 0,3,7,14 and 28days) and optionally 90 degree.
The route of administration of the vaccine is the intramuscular route: deltoid region (children: anterolateral aspect of thigh)
Some of Rabies related virus is (Lyssavirus genus)
- Serotype 1: Rabies virus
- Serotype 2: Lagos bat virus
- Serotype 3: Mokola virus
- Serotype 4:Duvenhage virus
- Serotype 6 & 7
- Australian bat lyssavirus
[embeddoc url=”https://notesmed.com/wp-content/uploads/2021/05/Rabies-virus.pdf” download=”all” cache=”off” text=”Complete pdf file-Download”]