What is necrosis?
Necrosis is defined as a series of changes that accompany cell death in living tissue, largely resulting from the progressive degradative action of enzymes on lethally injured cells in the body.
It is an “accidental” and unregulated form of cell death in the body. The acute inflammatory reaction occurs in the surrounding tissue.
Morphology
The general changes occurring in the necrotic tissue and cell:
- In the cytoplasm, there is increased eosinophilia. There are three patterns of nuclear changes,
- Pyknosis: It is a shrinkage of the nucleus which appears shrunken and deeply basophilic.
- Karyolysis: It is the progressive fading of basophilic staining of the nuclei and leads to ghost nuclei.
- Karyorrhexis: In the karyorrhexis, the nucleus breaks up into many smaller fragments of the nucleus.
The pattern of tissue necrosis (types):
- Coagulative
- Liquefactive
- Caseous
- Fat necrosis
- Fibrinoid necrosis
Coagulative necrosis
- It is characteristic of the area of infarcts (areas of ischemia) in all of the solid organs such as the heart, kidney, spleen, and limb (dry gangrene) except the brain. Ischemia is caused by an obstruction in a vessel.
- Mechanism: Ischemia denaturation and coagulation of enzymes and structural proteins.
- The preservation of the structural outline of dead cells in necrosis. It is the inactivation of intracellular enzymes that prevents the dissolution (autolysis) of the cell. eg. Myocardial infarction, renal infarction.
- Morphology:
- Gross: The affected tissue site takes on a firm texture, and it appears dry, pale, yellow. Some organs like the spleen and kidney are wedge-shaped.
- Microscopic examination: Eosinophilic, anucleate cells may persist and Leukocytes are recruited to the site of necrosis.
Gangrene (Gangrenous necrosis)
- It is a massive form with superadded putrefaction. Gangrenous usually refers to the condition of a limb of the body, generally the lower leg, that has lost its blood supply and has undergone coagulative necrosis involving multiple tissue layers. They are dry and wet gangrene.
- Dry gangrene:
- It predominantly consists of a coagulative type of necrosis. The affected site is dry shrunken (shriveled) dark brown or black resembling the foot of a mummy.
- In this dry gangrene, the demarcation line is clear & spread slowly but the prognosis is fair.
- It is caused by ischemia due to the fact that arterial obstruction & the rate of obstruction are slow.
- In wet gangrene:
- In this wet gangrenous when a bacterial infection is superimposed, then coagulative is modified by the liquefactive action of the bacteria and the attracted leukocytes resulting in is called wet gangrene.
- It is mostly caused by venous blockage (e.g. strangulated hernia, intussusception, or volvulus). The common site of wet gangrene is bowel, lung, mouth, etc.
- The affected part is soft, swollen, putrid, and dark but no clear demarcation. It is spread rapidly and the prognosis is poor due to severe septicemia.
Liquefactive necrosis
- The dead cells are transformed into a mass of liquid viscous due to the release of the enzymes from leukocytes accumulated at the site of necrosis.
- The dead tissue may rapidly undergo softening and transform into a liquid viscous mass.
- Causes:
- Focal bacterial or, occasionally, fungal infections.
- Hypoxic death of cells within the central nervous system (CNS) in the brain, eg. Infarct brain, Abscess.
- Mechanism: The dead cells are completely digested by the lysosomal enzymes released by neutrophils or dead cells(autolysis) and leukocytes (heterolysis), transforming the tissue into a liquid viscous mass (pus seen in case of acute inflammation). Pus consists of liquefied necrotic cell debris, macrophages (scavenger cells), and dead leukocytes.
Caseous necrosis
- It is encountered most often in foci of tuberculous infection and systemic fungal infection (e.g. histoplasmosis).
- It is due to the presence of a high amount of lipid in the cell wall in these organisms.
- Mechanism: Caseous material is composed of the release of lipid from the cell walls of Mycobacterium tuberculosis and systemic fungi after immune destruction by macrophages.
- Morphology:
- Grossly: The gross feature is the friable yellow-white appearance of the area(Caseous means “cheese-like,”)
- On microscopic examination: In this necrosis, the necrotic focus appears as a collection of a number of fragmented or lysed cells with an appearance of amorphous granular pink. It is undergoing dystrophic calcification.
Enzymatic Fat necrosis
- In enzymatic fat necrosis, fat destruction, typically resulting from the release of activated pancreatic lipases into the substance of the pancreas and the peritoneal cavity. eg. Traumatic fat necrosis in the breast, acute pancreatitis.
- Mechanism: Activation of pancreatic lipase (e.g. alcohol excess) causes hydrolysis of triglyceride in fat cells with a release of fatty acids. The conversion of fatty acids into soap (Fatty Acid+soap) (saponification).
- Morphology:
- Grossly: Chalky white areas of saponification.
- Histologic examination: In necrosis, the foci contain shadowy outlines of necrotic fat cells with basophilic calcium deposits, surrounded by an inflammatory reaction in this necrosis.
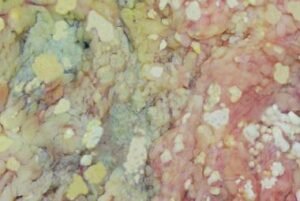
- Traumatic fat necrosis: It occurs in fatty tissue (for example, female breast tissue)due to a result of trauma. It is not enzyme-mediated.
- Fibrinoid necrosis:
- It was seen in immune reactions. The deposited immune complexes, together with fibrin that has leaked out of vessels, produce a bright pink and amorphous appearance on Hematoxylin and Eosin (H&E) stain preparations called fibrinoid necrosis (fibrin-like).
- For example, Autoimmune disease and peptic ulcer. It is mostly seen following immune-mediated diseases such as Polyarteritis nodosa, malignant hypertension, Aschoff bodies in rheumatic fever.


